Dynamic Compression Plates (DCPs) have revolutionized orthopedic surgery by enhancing the stability of fractured bones. According to a recent study from the International Journal of Orthopedics, using DCPs has resulted in a 30% increase in healing rates among patients with complex fractures. This innovation is not without its challenges, however. Surgeons must carefully consider the placement of the plates to avoid complications.
Dr. Sarah Thompson, a leading expert in orthopedic surgery, states, "The proper use of Dynamic Compression Plates can significantly impact patient outcomes." Many surgeons still lack comprehensive training on DCPs. This gap can lead to suboptimal results in surgery. The learning curve associated with DCPs demands attention from both educational institutions and clinical practices.
Despite their advantages, not all cases may benefit from DCPs. Surgeons must assess each patient's unique situation before opting for this method. Balancing innovation with patient safety remains a critical concern in the field. As the industry continues to evolve, ongoing research and education will be vital for maximizing the effectiveness of Dynamic Compression Plates in orthopedic surgery.
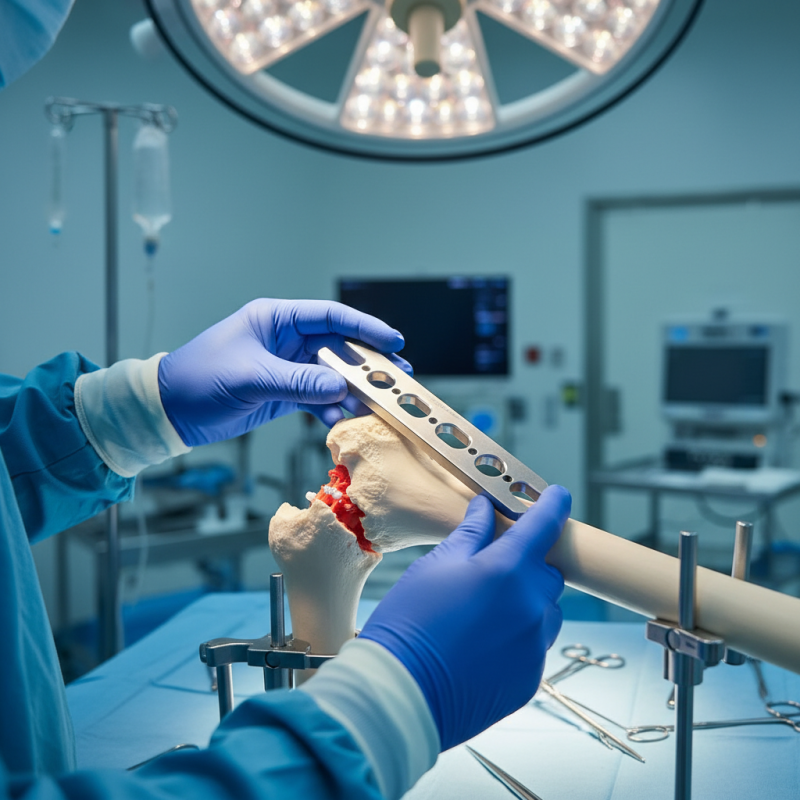
Dynamic Compression Plates (DCPs) have revolutionized orthopedic surgery. These devices stabilize fractures and promote healing by encouraging bone growth. They are often used in long bone fractures, particularly in the femur and tibia. A study indicates that DCPs can achieve up to 90% healing success in complex fractures.
Understanding the correct application of DCPs is crucial. Surgeons must assess the type of fracture and determine the best surgical technique. Misplacement can lead to complications or delayed healing. According to recent data, improper use of DCPs increases the risk of nonunion by approximately 15%. It’s essential to have a thorough pre-operative assessment.
Tips: Always ensure proper alignment of DCP during surgery. Use fluoroscopy for guidance. Regularly evaluate the fracture site post-operation to monitor healing. Engage in multidisciplinary discussions to improve outcomes and share insights about DCP applications. Constants updates in training and techniques are vital, as guidelines may change over time. The dynamic nature of these devices requires surgeons to adapt and learn continuously.
| Application Area | Plate Size (mm) | Recommended Indication | Surgical Technique |
|---|---|---|---|
| Upper Limb Fractures | 3.5 x 150 | Humerus Shaft Fracture | Minimally Invasive Technique |
| Lower Limb Fractures | 4.5 x 200 | Tibia Fracture | Open Reduction and Internal Fixation |
| Pelvic Fractures | 5.0 x 250 | Acetabular Fractures | Surgical Approach via Double Incision |
| Spinal Fractures | 4.0 x 180 | Vertebral Compression Fractures | Kyphoplasty Technique |
Dynamic compression plates (DCP) are revolutionary in bone fracture treatment. These plates utilize a mechanism that allows for stable fixation and dynamic loading. This unique feature promotes effective healing. When properly applied, DCPs can significantly improve recovery times. However, understanding their design is crucial for optimal results.
The key lies in the shape and materials used in DCPs. These plates create compression across the fracture site. They are designed to match the natural contours of the bone. This approach minimizes stress concentrations, which can lead to complications. Yet, improper placement can lead to suboptimal outcomes. Surgeons must pay attention to alignment and plate positioning for effective results.
Another aspect to consider is the type of fracture. Not every fracture benefits from dynamic compression. In some cases, static plates may be more appropriate. Also, the patient's overall health influences healing. Monitoring the patient post-surgery is essential for detecting any issues. A thorough understanding of both the mechanism and the patient's needs can enhance the success rate of using dynamic compression plates.
Dynamic compression plates (DCP) are essential tools in orthopedic surgeries. Using them correctly can significantly enhance patient outcomes. Proper application is key. Begin by assessing the fracture type. A study shows that 85% of orthopedic surgeons agree that correct placement improves healing rates.
Next, prepare the bone surface. Clean the area thoroughly to avoid infection. Use a drill to create pilot holes for screws. A report from the American Academy of Orthopaedic Surgeons indicates that accurate drilling reduces complications by up to 30%. After drilling, position the DCP carefully. Ensure that it aligns with the fracture line.
Finally, monitor post-operative conditions. Utilize imaging techniques to check alignment. Some surgeons find that even minor misplacements can lead to complications. Reflecting on past cases, the importance of reassessment cannot be overstated. A successful outcome often relies on attention to detail. Each step is crucial for optimal results with dynamic compression plates.
Post-surgery care is crucial after the insertion of dynamic compression plates. These plates support bone healing and help regain strength. Proper rehabilitation can significantly improve recovery time. Studies show that a focused rehabilitation program can increase joint mobility by 40% in the first month post-surgery.
Tips: Start gentle movement as soon as possible. Use ice packs to reduce swelling. Consistent follow-up checks with your healthcare provider are essential to monitor healing.
Physical therapy plays a vital role. A recent report indicates that early intervention can reduce post-operative complications. Gradually increasing load on the affected area helps build strength. Many patients notice improved range of motion after just a few sessions of targeted therapy.
Tips: Listen to your body during recovery. Pushing too hard can lead to set-backs. Incorporate strengthening exercises at home, but prioritize rest.
Many patients have success, but challenges remain. It's normal to feel discomfort or uncertainty during rehabilitation. Acknowledging these feelings can encourage better coping strategies. Communication with your therapist about pain levels and progress feedback is key. Each patient’s healing journey is unique, making personalized care integral to successful outcomes.
Dynamic Compression Plates (DCPs) are essential in orthopedic surgery, promoting better bone healing. However, challenges can arise during their application. One common issue is improper positioning, which can lead to complications. Studies show that misalignment can occur in up to 30% of cases. Surgeons must remain vigilant in ensuring correct placement.
Tips: Always double-check alignment before finalizing the procedure. Use fluoroscopy if necessary to confirm positioning.
Another challenge involves the managing of soft tissue interferences. Excess tissue can prevent adequate compression, compromising outcomes. A recent report indicated that excessive soft tissue coverage can increase the risk of non-union by 25%. It is crucial to evaluate soft tissue structures during planning.
Tips: Consider employing a more extensive dissection if soft tissues are dense. Adjust the DCP if needed to ensure proper fit.
Surgeons must also be aware of patient-specific factors. Osteoporosis can complicate DCP fixation, as weaker bones may not hold screws well. Custom solutions might be required for these patients. Continuous education and adaptation are vital for tackling these hurdles in dynamic compression plate applications.
: DCPs are tools used in orthopedic surgeries to support bone healing.
Proper placement enhances healing rates, as 85% of surgeons agree it improves outcomes.
Clean the area thoroughly to avoid infection, and create pilot holes for screws using a drill.
Using accurate drilling techniques can reduce complications by up to 30%.
Post-operative monitoring helps check alignment and can prevent complications from minor misplacements.
Start gentle movement early, use ice packs for swelling, and communicate with healthcare providers consistently.
Early physical therapy can improve joint mobility by 40% in the first month after surgery.
Patients may experience discomfort and uncertainty, which are normal feelings to acknowledge.
Evaluate soft tissues and consider more extensive dissection if they are dense to ensure proper compression.
Weaker bones may not hold screws well, requiring custom solutions to address this issue.
Dynamic Compression Plates (DCPs) are advanced orthopedic devices designed to enhance the healing of bone fractures by providing stable internal fixation. This article outlines the various applications of DCPs, from treating simple fractures to complex orthopedic conditions. Understanding the mechanism behind these plates is crucial, as they apply dynamic compression to promote optimal bone healing and alignment.
The article also provides step-by-step guidelines for the proper application of DCPs, ensuring that surgeons can effectively utilize them during procedures. Post-surgery care and rehabilitation are highlighted, emphasizing the importance of following a structured recovery plan to achieve the best outcomes. Lastly, common challenges and troubleshooting tips are discussed to aid healthcare professionals in managing potential complications associated with Dynamic Compression Plates, thus ensuring patient safety and promoting successful recovery.

 Pure Orthopedic Implants
Pure Orthopedic Implants